Parkinson’s disease is a progressive neurodegenerative disorder that profoundly impacts movement. It manifests through a range of symptoms including tremors, stiffness, and challenges with balance and coordination, further impacting mental health functioning and overall well-being of the individuals affected by the condition.
What is Parkinson’s Disease?
Parkinson’s disease is a chronic neurological condition 1 Zafar, S., & Yaddanapudi, S. S. (2019, February 11). Parkinson Disease. Nih.gov; StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470193/ characterized by the degeneration of specific brain areas, resulting in increasingly severe symptoms as the disease advances.
While the early symptoms of Parkinson’s disease are related to muscle control, balance, and movement, it can also have wide-ranging effects on sensory perception, cognitive function, mental health, and other aspects of well-being.
The prevalence of the disease varies across different regions, with an estimated 10 million 2 Ou, Z., Pan, J., Tang, S., Duan, D., Yu, D., Nong, H., & Wang, Z. (2021). Global Trends in the Incidence, Prevalence, and Years Lived With Disability of Parkinson’s Disease in 204 Countries/Territories From 1990 to 2019. Frontiers in public health, 9, 776847. https://doi.org/10.3389/fpubh.2021.776847 people affected globally. It is noteworthy that men have a higher risk of developing Parkinson’s compared to women, although women tend to experience a higher mortality rate and faster disease progression.
Although Parkinson’s disease typically manifests in older adults, usually around the age of 60 3 Camerucci, E., Stang, C. D., Hajeb, M., Turcano, P., Mullan, A. F., Martin, P., Ross, O. A., Bower, J. H., Mielke, M. M., & Savica, R. (2021). Early-Onset Parkinsonism and Early-Onset Parkinson’s Disease: A Population-Based Study (2010-2015). Journal of Parkinson’s disease, 11(3), 1197–1207. https://doi.org/10.3233/JPD-202464 , it can also affect younger individuals. When the onset occurs before the age of 50, it is referred to as young-onset 4 Post, B., van den Heuvel, L., van Prooije, T., van Ruissen, X., van de Warrenburg, B., & Nonnekes, J. (2020). Young Onset Parkinson’s Disease: A Modern and Tailored Approach. Journal of Parkinson’s disease, 10(s1), S29–S36. https://doi.org/10.3233/JPD-202135 Parkinson’s.
Signs and Symptoms of Parkinson’s Disease
Signs and symptoms of Parkinson’s disease can vary from person to person 5 Sveinbjornsdottir S. (2016). The clinical symptoms of Parkinson’s disease. Journal of neurochemistry, 139 Suppl 1, 318–324. https://doi.org/10.1111/jnc.13691 , but some common ones include:
1. Motor-related Symptoms
- Tremors: Uncontrollable shaking, often starting in the hands or fingers, and typically appearing at rest.
- Bradykinesia: Slowness of movement, making everyday 6 Bologna, M., Paparella, G., Fasano, A., Hallett, M., & Berardelli, A. (2020). Evolving concepts on bradykinesia. Brain : a journal of neurology, 143(3), 727–750. https://doi.org/10.1093/brain/awz344 tasks like walking, buttoning a shirt, or writing more challenging.
- Rigidity: Stiffness and resistance in muscles, leading to reduced flexibility and limited range of motion.
- Gait problems: Altered walking pattern, characterized by shuffling steps, decreased arm swing, and difficulty initiating or stopping movements.
- Drooling: Excessive saliva production due to impaired control of the muscles involved in swallowing and maintaining saliva in the mouth.
- Dysphagia: Difficulties with swallowing 7 Azer, S. A., & Kshirsagar, R. K. (2020). Dysphagia. PubMed; StatPearls Publishing. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559174/ , problems in eating and drinking, and increased risk of choking.
- Hypophonia: Reduced volume or softness of the voice 8 Hypophonia (Concept Id: C0521007) – MedGen – NCBI. (n.d.). Www.ncbi.nlm.nih.gov. Retrieved July 17, 2023, from https://www.ncbi.nlm.nih.gov/medgen/636383 , due to decreased muscle control in the vocal cords and respiratory muscles.
2. Non-motor Symptoms
- Autonomic dysfunction: Problems with regulating blood pressure, digestion, bladder control, and sexual function.
- Depression: Feelings of sadness, loss of interest, and worry, often accompanied by changes in appetite, sleep patterns, and energy levels.
- Loss of sense of smell (anosmia): A reduced ability to detect odors or a complete loss of the sense of smell is commonly observed in Parkinson’s disease.
- Sleep problems: Insomnia, excessive daytime sleepiness, restless leg syndrome, and vivid dreams or nightmares.
- Cognitive impairments: Some individuals with Parkinson’s may experience difficulties with thinking, memory, and focus.
- Emotional processing difficulties such as regulating emotions, mood swings, and difficulties in recognizing and expressing emotions appropriately with the situation.
Read More About Depression Here

How Parkinson’s Disease Impacts Mental Health
Parkinson’s disease can have a significant impact 9 Dommershuijsen, L. J., Van der Heide, A., Van den Berg, E. M., Labrecque, J. A., Ikram, M. K., Ikram, M. A., Bloem, B. R., Helmich, R. C., & Darweesh, S. K. L. (2021). Mental health in people with Parkinson’s disease during the COVID-19 pandemic: potential for targeted interventions?. NPJ Parkinson’s disease, 7(1), 95. https://doi.org/10.1038/s41531-021-00238-y on mental health functioning, such as:
- Anxiety, that leads to excessive worrying, restlessness, irritability, and fearfulness or panic symptoms.
- Depressive thoughts and feelings, which may include low mood, feeling of hopelessness, helplessness, and worthlessness.
- Stress, which arises from the demands of daily life tasks, unexpected events, ongoing problems, challenges, and uncertainties regarding the consequences of this disease.
- Anger, as the disease progresses and physical mobility issues increase, the feelings of frustration and temperament outbursts become more prominent.
- Loss of impulse control, difficulty in inhibiting inappropriate responses, or acting without considering the consequences.
- Apathy, which refers to a lack of motivation, interest, or initiativeness, can significantly impact a person’s engagement in daily activities and social interactions.
- Psychosis, which can involve hallucinations (seeing or hearing things that are not there) or delusions (holding false beliefs).
- Struggling to comprehend the potential consequences of the disease that can impact different facets of life, such as physical capabilities, daily routines, and future aspirations.
- Development of dementia, which involves signs of memory loss, confusion, and difficulties in thinking and reasoning.
Read More About Anxiety Here
What Causes Parkinson’s Disease
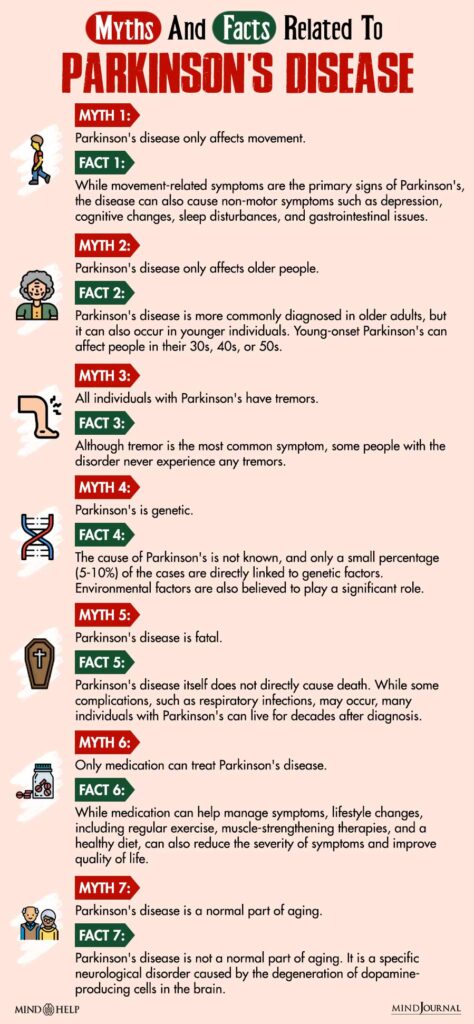
The exact cause of Parkinson’s disease is still not fully understood. However, several factors 10 Kouli, A., Torsney, K. M., & Kuan, W.-L. (2018). Parkinson’s Disease: Etiology, Neuropathology, and Pathogenesis. Parkinson’s Disease: Pathogenesis and Clinical Aspects, 3–26. https://doi.org/10.15586/codonpublications.parkinsonsdisease.2018.ch1 can develop Parkinson’s Disease, such as:
- Certain genetic mutations and variations are associated with an increased risk of developing Parkinson’s disease.
- Exposure to certain environmental factors and toxins such as pesticides, herbicides, industrial chemicals, etc.
- Older individuals over the age of 60, although young-onset Parkinson’s can also occur.
- Severe head injuries, particularly those resulting in loss of consciousness, are identified as a potential risk factor.
- Depletion of dopamine, a neurotransmitter involved in movement control.
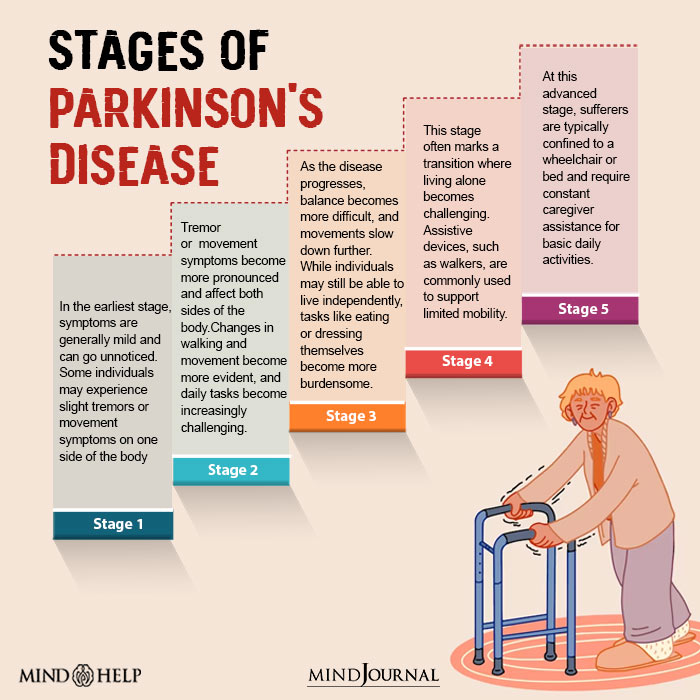
How to Diagnose Parkinson’s Disease
Parkinson’s disease diagnosis typically involves 11 Rizek, P., Kumar, N., & Jog, M. S. (2016). An update on the diagnosis and treatment of Parkinson disease. CMAJ : Canadian Medical Association journal = journal de l’Association medicale canadienne, 188(16), 1157–1165. https://doi.org/10.1503/cmaj.151179 a comprehensive evaluation by a healthcare professional, such as:
1. Medical History
Reviewing the affected individual’s medical history, including early symptoms of Parkinson’s disease along with progression, and family history. A thorough physical examination would be conducted, focusing on assessing motor symptoms, muscle stiffness, tremors, and balance issues.
2. Response to Medication
Parkinson’s disease symptoms often respond to certain medications that increase dopamine levels in the brain. A positive response to dopaminergic medication 12 Zahoor, I., Shafi, A., & Haq, E. (2018). Pharmacological Treatment of Parkinson’s Disease. Parkinson’s Disease: Pathogenesis and Clinical Aspects, 129–144. https://doi.org/10.15586/codonpublications.parkinsonsdisease.2018.ch7 , such as levodopa, can help support the diagnosis of Parkinson’s disease.
3. Neurological Examination
A neurological examination such 13 Spader, H. S., Grossberg, J. A., Haas, R. A., & Soares, G. M. (2013). Fundamentals of the neurologic examination for patients undergoing central nervous system interventional procedures. Seminars in interventional radiology, 30(3), 240–244. https://doi.org/10.1055/s-0033-1353476 as Computerised tomography, Magnetic resonance imaging (MRI), and Positron emission tomography (PET) scan may be performed to assess cognitive function, reflexes, muscle strength, coordination, and sensory abilities.
Treatment of Parkinson’s Disease
The treatment approach 14 Armstrong, M. J., & Okun, M. S. (2020). Diagnosis and Treatment of Parkinson Disease: A Review. JAMA, 323(6), 548–560. https://doi.org/10.1001/jama.2019.22360 can involve a combination of various strategies, including:
1. Medications
Various medications are 15 Sivanandy, P., Leey, T. C., Xiang, T. C., Ling, T. C., Wey Han, S. A., Semilan, S. L. A., & Hong, P. K. (2021). Systematic Review on Parkinson’s Disease Medications, Emphasizing on Three Recently Approved Drugs to Control Parkinson’s Symptoms. International journal of environmental research and public health, 19(1), 364. https://doi.org/10.3390/ijerph19010364 prescribed to help manage Parkinson’s symptoms, such as levodopa, dopamine agonists, MAO-B inhibitors, etc. These medications work by either increasing dopamine levels in the brain or improving dopamine function, helping to alleviate motor symptoms such as tremors, stiffness, and slow movement.
2. Deep Brain Stimulation (DBS)
Deep brain stimulation (DBS) is a surgical procedure 16 Fang, J. Y., & Tolleson, C. (2017). The role of deep brain stimulation in Parkinson’s disease: an overview and update on new developments. Neuropsychiatric disease and treatment, 13, 723–732. https://doi.org/10.2147/NDT.S113998 where electrodes are implanted in specific areas of the brain that control movement. These electrodes send electrical signals to those regions of the brain to help reduce the symptoms of Parkinson’s disease.
3. Physical Exercises
Physical exercise focuses on improving mobility, balance, and muscle strength. It can involve exercises, stretching, and techniques to enhance motor skills and ease movement difficulties.
4. Occupational Therapy
Occupational therapy helps individuals maintain independence in daily activities by providing strategies to manage motor challenges. This can involve techniques for dressing, eating, writing, and other activities of daily living.
Read More About Therapy Here
5. Speech Therapy
During speech therapy, exercises are done to improve the clarity of speech, learn techniques for swallowing, and develop strategies to overcome communication challenges.
6. Lifestyle Modifications
A healthy lifestyle, including a balanced diet, regular exercise, and sufficient rest, can support overall well-being and manage the symptoms.

Living with Parkinson’s Disease
Living with Parkinson’s disease requires a comprehensive approach 17 Pirtošek, Z., Bajenaru, O., Kovács, N., Milanov, I., Relja, M., & Skorvanek, M. (2020). Update on the Management of Parkinson’s Disease for General Neurologists. Parkinson’s disease, 2020, 9131474. https://doi.org/10.1155/2020/9131474 that integrates self-care, effective treatment management, and a strong support network. Regular physical exercise and a healthy lifestyle play pivotal roles in symptom management and overall well-being.
Adherence to medication schedules, along with open communication and collaboration with healthcare professionals, is essential for optimizing the treatment of Parkinson’s disease. Seeking support from loved ones, participating in support groups, and consulting with professional counselors can provide invaluable encouragement, guidance, and empowerment to individuals with Parkinson’s to gradually overcome challenges and lead fulfilling lives.
Takeaway
Parkinson’s disease is a complex neurodegenerative condition that affects movement and can have significant impacts on an individual’s physical and mental well-being. While there is no cure, early Parkinson’s disease diagnosis, proper management, and a multidisciplinary approach involving medication, therapy, and support can help individuals with Parkinson’s lead meaningful lives and optimize their quality of life.
At A Glance
- Parkinson’s disease is a progressive neurodegenerative disorder that profoundly impacts movement.
- The symptoms of Parkinson’s disease include motor-related and non-motor symptoms.
- Parkinson’s disease can have a significant impact on mental health functioning, such as anxiety, apathy, and psychosis.
- Several factors such as genetic variations, environment, and age play crucial roles in the development of Parkinson’s disease.
- Parkinson’s disease diagnosis typically involves a medical history, response to medication, and neurological examinations.
- Treatment for Parkinson’s disease typically involves a combination of medications, therapies, and lifestyle modifications.
Frequently Asked Questions (FAQs)
1. Is Parkinson’s disease hereditary?
Parkinson’s disease can have a hereditary component, but it is not always directly inherited. While certain genetic mutations and variations have been linked to an increased risk of developing Parkinson’s, the majority of cases occur without a clear genetic link.
2. Can you die from Parkinson’s disease?
Parkinson’s disease itself is not a direct cause of death, but its impact on the body can be significant. The condition can place considerable strain on individuals, potentially making them more susceptible to serious and life-threatening infections.
3. Is there a cure for Parkinson’s disease?
Although a cure for Parkinson’s disease has not yet been found, various treatment approaches including medications, surgical interventions, and other therapies can help alleviate and manage symptoms.















