Table of Contents
Sensory Processing Disorder (SPD) is a term that describes the difficulties in children (and adults) associated with their brain. Let us explore the various aspects of the disorder including diagnosis, treatment options and ways to cope with the condition.
What Is Sensory Processing Disorder?
Sensory processing disorder refers to a condition where the brain has trouble receiving and responding to a piece of information coming through the senses. In this condition, the child’s brain does not read the sensory messages he/she receives from their body completely. The condition can affect or interrupt the messages received to the brain from any of the senses.
People with this condition respond differently to such sensory information than normal people. Unlike people with hearing or sight impairment, SPD patients do detect the sensory information, however, since the sensory information gets “mixed up” in their brain, they are unable to come up with an appropriate response addressing the sensory information.
According to a study 1 Gourley, L., Wind, C., Henninger, E. M., & Chinitz, S. (2013). Sensory Processing Difficulties, Behavioral Problems, and Parental Stress in a Clinical Population of Young Children. Journal of child and family studies, 22(7), 912–921. https://doi.org/10.1007/s10826-012-9650-9 , a child’s ability to notice, organize and integrate information from a situation and his/her own body, followed by processing and appropriately responding to the same greatly contribute to self-regulation. However, issues with regulating sensory information such as touch, smell, taste, sound, body movement, or body position can lead to –
- Hypersensitivity to sensory stimuli or sensory-avoidance
- Hypo-sensitivity to sensory stimuli
- Sensory-seeking behaviours
- A mixed pattern of under-responsivity
- Sensory seeking and/or sensory avoidance
Formerly referred to as sensory integration dysfunction, sensory processing disorder (SPD) was not included in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) as a separate diagnostic category. However, sensory processing challenges are noted as one of the diagnostic criteria in autism.
Read More About DSM 5 Here.
Understanding Sensory Processing Disorder
Sensory processing theory was first defined by Dr. A. Jean Ayres 2 Guardado KE, Sergent SR. Sensory Integration. [Updated 2020 Jun 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559155/ in 1972 with the quest to distinguish those children who appeared to face difficulties integrating multiple sensory stimuli. The theory was developed to explain the relationship between deficits in interpreting sensory stimuli from the sensation body & the environment and difficulties with academic or motor learning.
According to a study, sensory processing challenges are neurologically-based problems. The difficulty originates from the brain’s inability to combine the sensory messages it receives from the sensory systems and turn the input into practical responses. The disorder affects sight, smell, sound, touch, body position, and movement individually or in combination.
Sensory processing issues are usually recognized during the toddler years. During this period, the parents observe the child’s unusual aversion to light, noise, shoes that are considered too tight and clothes that are disturbing. They may also notice clumsiness and trouble climbing stairs backed by a struggle connected to fine motor skills like fastening buttons or using a pencil. The condition becomes alarming or baffling to parents when children display extreme behaviors such as:
- Screaming upon their faces getting wet
- Throwing tantrums while getting them dressed
- Suffering an odd high or low pain threshold
- Bumping into walls and even people
- Putting inedible things such as rocks and paint into their mouths
Additionally, sensory processing problems are now considered a symptom of autism because the majority of children and adults on the autism spectrum also have significant sensory issues. In fact, according to a study 3 Pfeiffer, B. A., Koenig, K., Kinnealey, M., Sheppard, M., & Henderson, L. (2011). Effectiveness of sensory integration interventions in children with autism spectrum disorders: a pilot study. The American journal of occupational therapy : official publication of the American Occupational Therapy Association, 65(1), 76–85. https://doi.org/10.5014/ajot.2011.09205 , sensory processing disorder (SPD) is quite common among children with ASD backed by a prevalence rate of 42% to 88%.
Prevalence Of Sensory Processing Disorder
”Most epidemiological studies carried out in western-lifestyle populations indicate a surprisingly high prevalence of SPD among children” explains a study 4 Galiana-Simal, A., Vela-Romero, M., Romero-Vela, V. M., Oliver-Tercero, N., García-Olmo, V., Benito-Castellanos, P. J., Muñoz-Martinez, V., & Beato-Fernandez, L. (2020). Sensory processing disorder: Key points of a frequent alteration in neurodevelopmental disorders. Cogent Medicine, 7(1). https://doi.org/10.1080/2331205x.2020.1736829 . The researchers found that 13.7% of 3 to 6 years children met the diagnostic criteria of SPD. It has also been observed that American boys and girls aged 3 to 10 years had 11.6% of SPD prevalence.
A 2009 study 5 Gouze, K. R., Hopkins, J., LeBailly, S. A., & Lavigne, J. V. (2009). Re-examining the epidemiology of sensory regulation dysfunction and comorbid psychopathology. Journal of Abnormal Child Psychology, 37(8), 1077-1087. https://doi.org/10.1007/s10802-009-9333-1 found that boys were more likely to have SPD than girls with a prevalence rate of 14.6% vs 8.6% respectively. It was also observed that 63% of SPD sufferers tend to have a psychiatric disorder while 37% did not have any other disorders, establishing that SPD exists independently of psychiatric conditions. The study concluded that the prevalence of “pure” SPD was approximately around 5%. Another study 6 Engel-Yeger, B. (2010). The applicability of the short sensory profile for screening sensory processing disorders among Israeli children. International Journal of Rehabilitation Research, 33(4), 311-318. https://doi.org/10.1097/mrr.0b013e32833abe59 showed that 15% out of 395 boys and girls across Israeli schools met the criteria of SPD.
What Is Sensory Information?
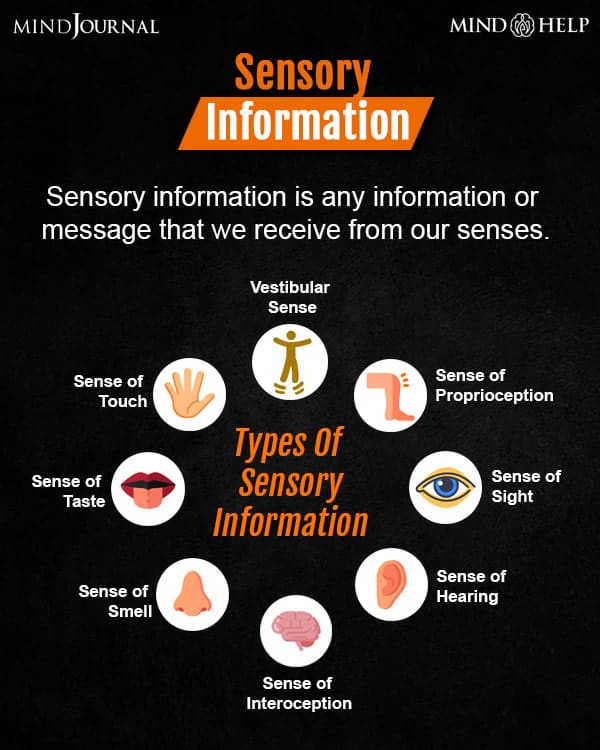
Sensory information is any information or message that we receive from our senses. This includes the five common senses- the sense of taste, the sense of smell, the sense of sight, the sense of hearing, and the sense of touch. Additionally, we receive directions from our proprioceptive and vestibular senses. Here are the eight types of sensory information that we receive from various sensory organs.
1. Sense of Taste
We can relate to the sense of taste when we receive information from the tongue. Such information usually comes from various food flavours such as sweet, sour, salty, and savoury flavours. It’s also called gustatory sense.
2. Sense of Smell
The nose receives sensory messages from perfume, food, smoke, flowers, etc. It is also known as olfactory sense 7 Purves D, Augustine GJ, Fitzpatrick D, et al., editors. Neuroscience. 2nd edition. Sunderland (MA): Sinauer Associates; 2001. The Organization of the Olfactory System. Available from: https://www.ncbi.nlm.nih.gov/books/NBK10982/ .
3. Sense of Sight
Sense of sight operates when our eyes receive sensory messages from sensory input like colors, object movement, distance, shapes, or anything which we can view.
4. Sense of Hearing
Also known as auditory sense, the ear receives these sensory messages in the form of sound waves. Examples of such sensory input include child crying, a vacuum cleaner, an alarm, mobile ringtone, music playing, etc.
5. Sense of Touch
The touch or tactile sense receives sensory messages from the skin. In addition to touch, this includes information about temperature, pain, and pressure/vibration.
6. Sense of Proprioception
Our proprioceptive sense is extremely vital and it is often addressed as the hidden sixth sense. It receives sensory messages from our muscles and joints. Such messages help us understand the working of our limbs along with the amount of force we are using during physical activity. Some example activities that give a lot of proprioceptive feedback are squeezing an orange, pushing a pram or a stroller, cycling, etc.
7. Vestibular Sense
The vestibular sense is often called the balance sense and it receives sensory instructions from the inner ear part called the vestibule. The vestibular sense promotes balance and coordination of movement along with alertness. Research 8 Guardado KE, Sergent SR. Sensory Integration. [Updated 2020 Jun 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559155/ reveals that vestibular receptors develop early in fetal development and are functioning at birth. The vestibular system feeds the brain with critical information regarding velocity and direction of head movement and static head position relative to gravity.
8. Sense of Interoception
Interoception refers to the messages we receive from our internal organs. This includes internal pain along with information about hunger, fatigue and needs to use the toilet.
Types Of Sensory Processing Disorder
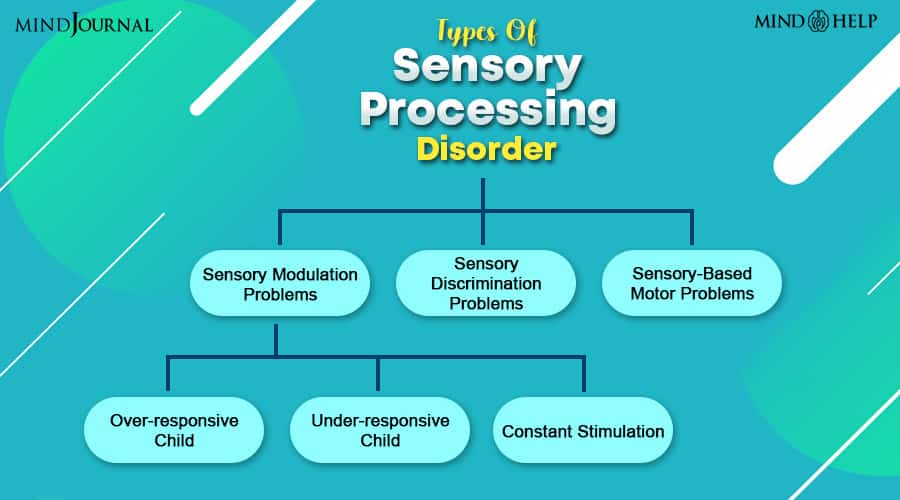
The sensory processing disorder can be divided into the categories mentioned below:
1. Sensory Modulation Problems
Troubles with movement, touch, and body position are significant signs of SPD. This is further divided into three major categories, such as –
A. Over-responsive Child
This condition is defined by a situation where the child seeks less stimulation, i.e., avoids touching or being touched, moving or being unexpectedly moved. The child may also be firm and uncoordinated.
B. Under-responsive Child
Unlike the previous condition, an under responsive child seeks more stimulation. He/she may be oblivious of messy hands, or clothes. The child may be unable to feel things, along with a lack of inner drive to move objects or play. However, children with this condition become extra alert after pushing, pulling, or lifting.
C. Constant Stimulation
This condition of SPD is defined by a situation where the sensory craver seeks stimulation. This may include activities like rolling in mud, searching purposelessly through toys, constantly rubbing against walls and bumping into people. The child may also crave for fast movement, gets into upside-down positions along with displaying atypical ways to smell, sight, sound, and taste.
2. Sensory Discrimination Problems
Another category of SPD is Sensory Discrimination Disorder. This condition is defined by a situation in which the child finds it difficult to differentiate between one sensation and another, or in reading a particular sensation. Children may have trouble with touch, body movement and position, balance, sight, muscle control, sounds and taste.
3. Sensory-Based Motor Problems
This category of SPD includes two conditions. One is known as Postural Disorder, i.e., difficulties with movement patterns, bilateral coordination and balance. The second one is known as Dyspraxia which involves problems associated with coordinated and voluntary actions, including both fine and gross motor planning.
Symptoms Of Sensory Processing Disorder

Sensory processing disorder can affect one or multiple senses. Children who suffer from this disorder may have an exaggerated reaction towards sounds, clothing, and food textures. They may also underreact to sensory input. This condition, in turn, leaves them with more craving for intense thrill-seeking stimuli. Examples of such activities include swinging too high or jumping off tall things on the playground. Additionally, a child with SPD may be both oversensitive and under-sensitive towards day to day activities.
1. Symptoms of Over Sensitiveness or Sensory Avoiding
Children who are oversensitive or have sensory avoiding conditions may react to a wide range of triggers. You may find a child with SPD with the oversensitive condition when he/she:
- Thinks apparel are too scratchy or itchy
- Thinks the light is too bright
- Thinks sounds appear too loud
- Believes soft touches feel too hard
- Experience a sense of choking with food textures
- Have poor balance or look clumsy
- Are afraid to play on the swings
- React inadequately to unexpected movements, loud noises, touches, or bright lights
- Have behavior problems
- Gets easily overwhelmed by people or places
These symptoms are at times also associated with poor motor skills. A child may find it difficult to hold a pen, pencil or scissors. He or she may struggle with climbing stairs or have low muscle tone along with language delays. In older children, these symptoms may lead to low self-confidence resulting in social isolation and even depression.
2. Symptoms of Under Sensitiveness or Sensory Seeking
On the contrary, children with under-sensitiveness or sensory-seeking condition may exhibit the following signs:
- Unable to sit still
- Seek thrills through activities such as jumping, spinning and height
- Spin continuously without feeling
- Don’t pick up on social cues
- Do not understand the concept of personal space
- Chew on things including their hands and clothing
- Seek visual stimulation
- Have problems with sound sleep
- Do not understand when their face is dirty or nose is running
- Has a high tolerance for pain
- Clumsy and uncoordinated
However, it must be noted that kids do not always stick to a particular category of SPD. A child may be sensory seeking in certain situations and sensory avoiding in others. It entirely depends on the coping or self-regulating pattern of the child at that time. Thus, it is extremely important for the parents to observe their child’s reactions while trying to predict what triggers them.
Causes Of Sensory Processing Disorder
Health experts and professionals are yet clear about the factors that cause sensory issues in children or sensory processing disorder. Additionally, some professionals and researchers are not yet clear whether it can occur on its own or not while others believe it to be a symptom of another issue, not its own issue.
A 2006 study 9 Goldsmith, H. H., Van Hulle, C. A., Arneson, C. L., Schreiber, J. E., & Gernsbacher, M. A. (2006). A population-based twin study of parentally reported tactile and auditory defensiveness in young children. Journal of Abnormal Child Psychology, 34(3), 378-392. https://doi.org/10.1007/s10802-006-9024-0 involving twins concluded that hypersensitivity to light and sound may be because of the genetic component. It was assumed that if one twin was extremely sensitive, the other twin was likely to suffer the same condition. The same study had also reported that children who are afraid or anxious may display sensory processing disorder when dealing with physical stimuli like brushing hair. Apart from the possible genetic connection, sensory issues may also occur in prematurely born children or ones who had experienced birth complications.
Diagnosis Of Sensory Processing Disorder
Since sensory processing disorder is not perceived as an official condition, there are no formal criteria for the diagnosis. Instead, doctors, educators, or healthcare providers who work with children with SPD give out information about the child’s behaviors and interactions.
Since these sensory issues are highly visible, it makes the diagnosis easier. However, there are a few tests such as the Sensory Integration and Praxis Tests 10 Mailloux, Z. (1990). An overview of the sensory integration and praxis tests. American Journal of Occupational Therapy, 44(7), 589-594. https://doi.org/10.5014/ajot.44.7.589 (SIPT) or the Sensory Processing Measure 11Jorquera-Cabrera, S., Romero-Ayuso, D., Rodriguez-Gil, G., & Triviño-Juárez, J. M. (2017). Assessment of Sensory Processing Characteristics in Children between 3 and 11 Years Old: A Systematic Review. Frontiers in pediatrics, 5, 57. https://doi.org/10.3389/fped.2017.00057 (SPM) that can help the healthcare providers and educators to understand a child’s sensory function better.
Additionally, occupational therapists (OTs) are often considered qualified enough to recognise and plan treatment for children with sensory challenges. Other professionals who are able to identify sensory processing issue are:
- Pediatricians
- Developmental-Behavioral Paediatricians 12 Blum, Nathan J. MDthe DBPNet Steering Committee The Developmental-Behavioral Pediatrics Research Network: Another Step in the Development of the Field, Journal of Developmental & Behavioral Pediatrics: January 2012 – Volume 33 – Issue 1 – p 78-83 doi: 10.1097/DBP.0b013e31823e05bb
- Psychologists, including neuropsychologists
- School evaluators
Additionally, parents must observe their child’s behavior and reaction to better identify the behavior patterns and triggers. As someone who stays with their child 24×7, they are the first and the best observers of a child’s day to day behavior or reactions.
When To See A Doctor
If you suspect that your child has sensory processing disorder, these symptoms may indicate that it’s time to consult a doctor.
- When the behavior of your child disrupts his/her everyday life, thereby making it difficult to carry a normal day
- When the symptoms take a dramatic turn
- When it becomes beyond normal to manage the reactions of your child
While parents may recognize abnormalities in their child’s, they may not understand the reason behind such developments. Thus, rather than being afraid, they must consult an expert who can assess their child with SPD. The therapist will ask a few questions and everything will take forward the diagnosis.
Treatment Of Sensory Processing Disorder
Currently, there are no medications curated to deal with a sensory processing disorder. However, there are professionals or experts who can help a child learn tactics to cope with sensory challenges. Treatment for Sensory Processing Disorder is usually done through therapies by the experts. Also, it is recommended to start the therapies early as it is the key to treating SPD. The various therapies can help a child learn how to manage their challenges.
The therapy sessions are done by trained therapists who will first learn the condition of your child,which is whether he/she falls under the oversensitive category, under-sensitive category, or a combination of both. The different types of therapies are as given below:
1. Sensory Integration Therapy (SI)
This type of therapy is defined by playful activities in a controlled and safe environment. The therapist will enable a child to experience stimuli without feeling overwhelmed. He or she can also improve coping skills for dealing with that stimuli. Through this therapy, coping skills can become an everyday response to stimuli.
SI is designed to help a child learn how their experiences differ so they can accurately assess a more expected response. According to a study 13 Section On Complementary And Integrative Medicine; Council on Children with Disabilities; American Academy of Pediatrics, Zimmer M, Desch L. Sensory integration therapies for children with developmental and behavioral disorders. Pediatrics. 2012 Jun;129(6):1186-9. doi: 10.1542/peds.2012-0876. Epub 2012 May 28. PMID: 22641765. , occupational therapy coupled with sensory-based therapies is accepted as one of the components of a comprehensive treatment plan.
2. Occupational Therapy
An occupational therapist is assigned to work with a child to help him/her with other symptoms related to SPD. Occupational therapy can help a child with fine motor skills, using scissors, holding a pen or a pencil, handwriting, etc. Additionally, the therapy can also help a child to enhance gross motor skills such as climbing stairs and throwing a ball to name a few. It can also teach everyday skills like getting dressed, combing hair, etc.
3. Sensory Diet Therapy
Many times, sensory diet therapy will enhance other SPD therapies. However, it must be noted that it is not associated with a typical food diet but sensory activities for home and school. These activities are created to support a child to stay focused and arranged during the day. Sensory diet therapy is tailor-made based on a child’s needs. A sensory diet at school might include activities such as:
- Scheduling a particular time every hour for a child to go for a 10-minute walk
- Setting up a time twice a day when a child can swing for 10 minutes
- Allow in-class headphones that will enable a child to listen to music while working
- Using fidget toys
- Give a child the access to a desk chair bungee cord that will help one to move his or her legs while sitting in the classroom.
4. Cognitive Behavioral Therapy (CBT)
Child psychologists also work with children who have sensory processing disorder. They can use cognitive behavioral therapy 14 Rathod, V. J., Shah, V., Alagesan, J., Paranthaman, P., & P, S. (2015). Effect of sensory integration therapy and cognitive behavioral therapy on attention deficit hyperactivity disorder: Single blinded study. International Journal of Physiotherapy and Research, 3(2), 947-954. https://doi.org/10.16965/ijpr.2015.112 to enable kids to talk about their feelings, experiences and frustrations caused by their challenges.
Read More About Cognitive Behavioral Therapy Here.
5. Developmental, Individual Difference, Relationship Therapy
There is yet another type of therapy, known as the Developmental, Individual Difference, Relationship-based therapy or DIR model. It was designed by Stanley Greenspan, MD, and Serena Wieder, PhD and the key element of this therapy is the “floor-time” method. In simpler words, the DIR model involves multiple play sessions with the child and parent. The play sessions last for about 20 minutes. The therapy is divided into two parts.
A. First Part
In the first part of the session, the parents are asked to follow the child’s behavior, even if the pattern isn’t typical. This way, the parents can place themselves in their child’s position.
B. Second Part
In the second phase, the parents use the play session to create challenges for the child. The challenges enable to put the child into what Greenspan calls a “shared” world with the parent. Such challenges help the child master important skills in areas such as:
- Thinking
- Relating
- Communicating
If left untreated, SPD will remain a lifelong problem meddling with the child’s friendships, capacity to learn, and with the communication and coping skills of everyone in the family.
Risk Factors For Sensory Processing Disorder
The possible risk factors associated with SPD may involve the following:
- Prematurity (less than 36 weeks gestation)
- Maternal stress
- Low birth weight (less than 2200 gram)
- Maternal ailment
- Prenatal complexities
- Maternal use of medicines
- Assisted delivery methods
- Ethnic minority
- Childbirth complications
- Dwelling with a single parent
- Lower socioeconomic status
Helping A Child With Sensory Processing Disorder
Dealing with your child suffering from sensory processing disorder can be hard on the whole family. However, upon learning the cause behind the disorder, it gets simpler to know how to help your child. There are a few coping and self-help strategies that can be utilized to help your child, such as:
1. Bath Time
Activities associated with the bath time can help your child with SPD symptoms. For example, scrub his/her body with a washcloth or bath brush. Allow him/her to play on the wall with shaving cream or bathing foam. Let him/her apply body wash followed by rubbing body lotion after bath time.
2. Kitchen Activity
If you are fond of baking, involve your child in the same activity. Let your child mix elements, especially the thick ones that will foster the work of those muscles. Allow your child to mix, roll the dough and push flat. Additionally, tell your child to help you with carrying pots, pans and bowls of water to facilitate muscle movement.
3. Grocery Shopping
Let your child push the heavy cart along with carrying heavy products and putting them away.
4. Mealtime Activity
Tell your child to eat chewy foods while drinking out of a straw. Help your child sit on an air cushion to foster some movement.
5. Household chores
Let your child help you in various household chores such as assisting with vacuuming or furniture movement. from laundry to gardening, make sure to involve your child in all the possible household activities devoid of any risk.
6. Playtime Activities
From reading storybooks in the rocking chair to listening to soft music, from swimming in the pool to jumping on trampolines, taking part in horse riding and bowling, encourage your child into all those activities that will foster muscle movement.
Note For Caregivers/Parents
It is also essential for the parents to take care of themselves as the entire situation of dealing with a child with SPD can be very exhausting. Apart from working on your patience and mental strength, here are the other things that you should do as well:
- Listen to what the other parents with the same condition at home have to say and follow their advice if suitable
- Connect and trade tips with other parents
- Reach out to experts or therapists with whom you can discuss your mental condition
- You can also hire a separate caregiver who can take care of your child, thereby leaving you with some time to relax and indulge in your hobbies
Seek Professional Help
Our senses play a major role in organizing our day to day life as it tells us a lot about the world revolving around us. If you see your child struggling to gather and interpret those sensory inputs, it is better to consult a doctor as it may indicate the presence of sensory processing disorder. While treatments won’t be able to provide a complete cure for the condition, it will reduce exaggerated reactions and find healthier ways to cope with these sensory experiences.
Sensory Processing Disorder At A Glance
- Sensory Processing Disorder (SPD) is a term that describes the difficulties in children (and adults) associated with their brains.
- SPD refers to a condition where the brain has trouble receiving and responding to a piece of information coming through the senses.
- Sensory processing issues are usually recognized during the toddler years.
- Sensory information is any information or message that we receive from our senses.
- Sensory processing disorder can affect one or multiple senses
- Treatment for SPD is usually done through therapies by experts.















