Restless legs syndrome is a nervous system disorder characterized by a persistent and continuous urge to move one’s legs. It is also known as Willis Ekbom disease.
What is Restless Legs Syndrome (RLS)
Restless Legs Syndrome occurs when an individual experiences constant twitchiness and discomfort in their legs, usually after going to bed. Mind Help defines this condition as a “generic sensorimotor neurological disorder of the nervous system. It can lead to a severe and uncontrollable desire to move one’s legs constantly and unnecessarily.” Symptoms of this condition usually tend to occur in the late afternoon or early evenings and become more severe at night.
This condition can be classified as mild or severe, depending on the severity and frequency of the symptoms. It usually occurs when the person is resting such as sitting or lying in bed. It can also occur when a person is inactive and sitting for an extended period of time like watching a movie or sitting on a plane. The individual tends to feel constant discomfort and an urgent need to move their legs when they are idle.
“The non-painful but strong perceived need to move their legs when their legs are at rest is relieved with leg motion. There is a diurnal pattern wherein symptoms worsen at night, and sleep disturbance is often a problem,” explains a research paper 1 Mansur A, Castillo PR, Rocha Cabrero F, et al. Restless Leg Syndrome. [Updated 2020 Oct 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430878/ . People with this condition often find it difficult to fall asleep or go back to sleep after waking up.
The movement of the legs tends to ease the discomfort they feel. RLS is classified as a “sleeping disorder” since the symptoms are triggered while resting or attempting to sleep and a “movement disorder” due to the urgency to move the legs to relieve the symptoms. Research 2 Cuellar NG. Advances in the science of genomics in restless legs syndrome. Biol Res Nurs. 2010 Oct;12(2):178-87. doi: 10.1177/1099800410363168. PMID: 20453019. shows that around 15% of the global population is affected by RLS.
Understanding Restless Legs Syndrome
This condition can cause exhaustion and daytime sleepiness which ultimately can interfere with school or work performance and even personal relationships. People with this condition often report being unable to concentrate, are moody, have impaired memory, or fail to accomplish daily tasks. The individual tends to move their legs repeatedly in order to relieve the symptoms.
If moderate or severe RLS is left untreated, it can lead to a 20 percent decrease in work productivity. It can also contribute to depression or anxiety. The lack of sleep eventually leads to mood swings, irritability, compromised immune systems, and other physical health problems.
This condition can occur in both men and women. However, women are more susceptible to Restless Legs Syndrome or RLS than men. People who are affected are usually middle-aged or older. The symptoms tend to become more frequent with age. It is worth mentioning that most cases are treatable with non-drug therapies and if necessary, medications are prescribed.
In case RLS is triggered by a condition, illness, pregnancy, or medication, it may go away as soon as the triggering agent is gone. Sometimes cutting back or eliminating caffeine, alcohol, and tobacco can help ease the symptoms. Some people can even try massaging their legs while taking a warm shower to minimize the symptoms.
Estimates suggest that 7 to 10 percent of the US population have this condition. Studies3 Guo, S., Huang, J., Jiang, H., Han, C., Li, J., Xu, X., Zhang, G., Lin, Z., Xiong, N., & Wang, T. (2017). Restless Legs Syndrome: From Pathophysiology to Clinical Diagnosis and Management. Frontiers in aging neuroscience, 9, 171. https://doi.org/10.3389/fnagi.2017.00171 suggest that the prevalence rate of this condition is between 3.9 percent to 15 percent. Reports 4 Restless legs syndrome. (2017). nhs.uk. https://www.nhs.uk/conditions/restless-legs-syndrome/ found that 20 percent of women experience this condition during the last trimester of pregnancy. A review found that 1 in 10 people are affected at some point in their life.
Signs And Symptoms Of Restless Legs Syndrome
The primary signs and symptoms are an urge to move their legs. It usually happens on both sides of the body. It does not commonly affect the arms. “The symptoms occur at rest, are relieved by movement, and usually worsen in the evening,” states a 2014 study 5 Srivanitchapoom, P., Pandey, S., & Hallett, M. (2014). Restless legs syndrome and pregnancy: a review. Parkinsonism & related disorders, 20(7), 716–722. https://doi.org/10.1016/j.parkreldis.2014.03.027 . Common accompanying symptoms are as follows:
1. Sensations begin after rest
The sensations tend to begin after the individual is lying down or sitting for an extended period of time such as in a car, airplane, or movie theater.
2. Relief with movement
The sensations tend to lessen with the movement, such as stretching, jiggling your legs, pacing, or walking.
3. Worsening of symptoms in the evening
Symptoms usually occur as the night progresses. The sufferer may feel a stronger urge to move their legs later in the evening or at night. It has been observed that a symptom-free period usually occurs in the morning.
4. Leg twitching at night
It may be associated with another more common condition called periodic limb movement of sleep that causes the legs to twitch and kick throughout the night or while sleeping.
RLS And Periodic Limb Movement Of Sleep (PLMS)
This condition is closely associated with Periodic Limb Movement of Sleep. PLMS is a condition characterized by the incessant need to twitch or jerk one’s legs during sleep that occurs every 15 secs to 40 secs. This can also occur throughout the night. More than 80 percent 6 Joseph V, Nagalli S. Periodic Limb Movement Disorder. [Updated 2020 Jul 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK560727/ of people tend to experience periodic limb movement of sleep. Even though individuals with RLS tend to develop PLMS, vice versa is not necessarily the case. This can cause the individual to wake up frequently during the night. This, in turn, can cause poor quality and length of sleep.
What Restless Leg Syndrome Feels Like?
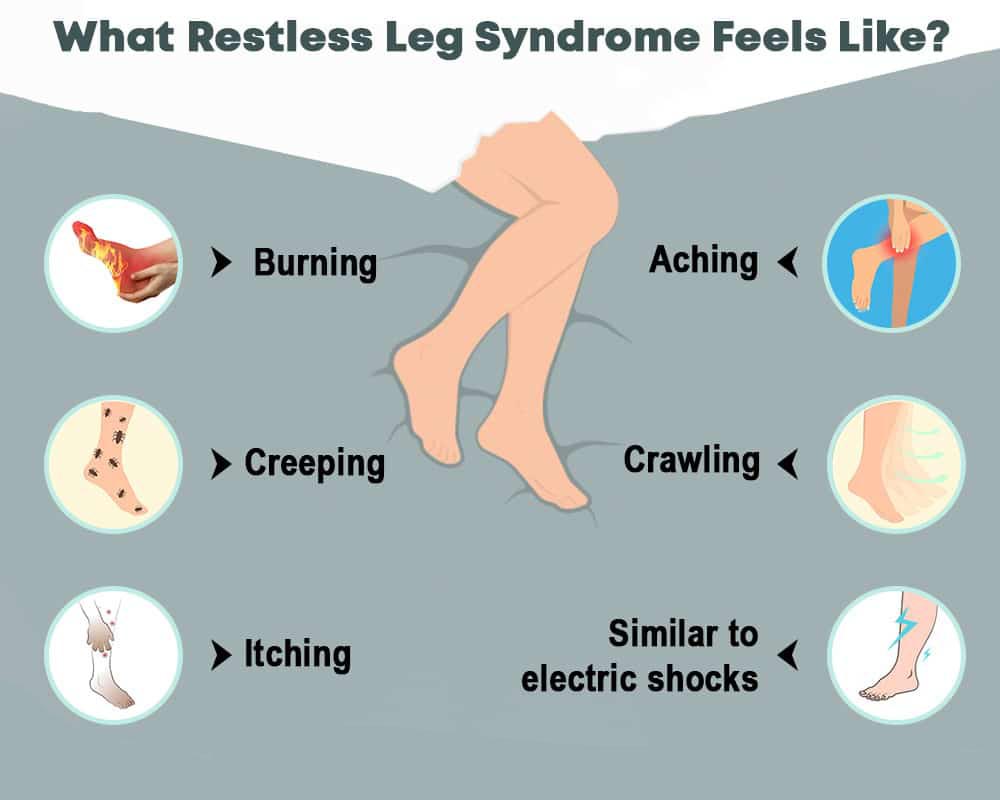
An individual with this condition has a strange and unpleasant sensation in the legs and sometimes the arms and a strong urge to move them. People usually describe these feelings as:
- Aching
- Burning
- Crawling
- Creeping
- Similar to electric shocks
- Itching
- Tugging
- Tingling
The only way to ease the discomfort is by moving the legs. The sensation tends to occur when the individual is resting or inactive. Symptoms tend to worsen in the evening and even more at night and maybe relieved for a short span in the morning.
Relationship Between Pregnancy And RLS Symptoms
Women often experience the symptoms of this syndrome during pregnancy. Women who already have this condition can experience the symptoms to get worse. The symptoms worsen as the pregnancy progresses, especially in the third trimester. According to a 2015 study 7 Gupta, R., Dhyani, M., Kendzerska, T., Pandi-Perumal, S. R., BaHammam, A. S., Srivanitchapoom, P., Pandey, S., & Hallett, M. (2016). Restless legs syndrome and pregnancy: prevalence, possible pathophysiological mechanisms and treatment. Acta neurologica Scandinavica, 133(5), 320–329. https://doi.org/10.1111/ane.12520 , “RLS during pregnancy has also been found to be associated with sleep disturbances, insomnia and early morning awakenings.” The study found that RLS-associated sleep disturbances can negatively affect pregnancy. The cause of the increased incidence of the condition during pregnancy is unknown. However, experts believe that the following factors may contribute to the condition:
- Low levels of minerals and vitamins such as iron and folate
- Sleep deprivation
- Hormonal changes
- Increased sensitivity in all the five senses
Pregnant women may not respond to the drugs prescribed. Research on the effectiveness of drugs for RLS in pregnant women is limited. The primary treatment methods that are followed for pregnant women are mild exercises and a healthy sleeping pattern. In case low iron levels are the cause of this condition, they may be prescribed iron supplements. In severe cases, it may be done intravenously. In extreme cases, if there is a different cause and the patient doesn’t respond to the treatment methods, then medication may be prescribed in low doses.
Types Of Restless Legs Syndrome
There are usually two types of RLS. They are as follows:
1. Primary or idiopathic RLS
Symptoms may be sporadic or can gradually worsen and become more prevalent over time. It is the most common type and its characteristic are as follows:
- It usually begins before the age of 40
- It can start as early as childhood
- It may have a genetic cause
- Primary RLS tend to be lifelong
2. Secondary RLS
Secondary Restless Legs Syndrome is usually caused by another condition or disease. The exact cause of this condition is unknown. However it may be related to how the body processes dopamine, a neurotransmitter responsible for controlling muscle movements. One 2009 study 8 Oka Y, Ioue Y. [Secondary restless legs syndrome]. Brain Nerve. 2009 May;61(5):539-47. Japanese. PMID: 19514514. states “Secondary RLS usually occurs later in life and in the absence of a family history of RLS.” Diagnosis can be challenging, especially in sufferers with neurological comorbidities. The most common characteristics are as follows:
- It usually starts after the age of 45 years
- It does not tend to be hereditary
- Onset is sudden
- Symptoms do not worsen over time
- Symptoms may be more severe
The diseases and symptoms that can trigger the symptoms:
- Diabetes
- Iron deficiency
- Kidney failure
- Parkinson’s disease
- Neuropathy
- Pregnancy
- Rheumatoid arthritis
Causes Of Restless Legs Syndrome

According to research 9 Massey, T. H., & Robertson, N. P. (2020). Restless legs syndrome: causes and consequences. Journal of neurology, 267(2), 575–577. https://doi.org/10.1007/s00415-019-09682-6 , the following factors or underlying conditions may be responsible for developing this condition:
- Genetic components can be found in families. Certain gene variants have been associated with this condition
- Dysfunction in one of the sections of the brain called basal ganglia, that controls movement that uses a brain chemical called dopamine.
- Individuals with Parkinson’s disease that causes disruption in the basal ganglia have an increased chance of this condition
- End-stage renal disease and hemodialysis
- Iron deficiency
- Medications such as anti-nausea drugs, antipsychotic drugs, antidepressants that increase serotonin
- Use of alcohol, nicotine, and caffeine
- Pregnancy especially in the last trimesters
- Neuropathy (nerve damage)
- Sleep deprivation or other sleep disorders
- Lesions on the spinal cord due to damage or injury
Read More About Insomnia Here
How Restless Legs Syndrome Diagnosed?
There is no specific test for diagnosing this condition. The condition is diagnosed by a doctor’s evaluation. The five basic criteria for clinically diagnosing this disorder are:
- A strong and frequent overwhelming need or urge to move the legs is often associated with abnormal, unpleasant, or uncomfortable sensations.
- The urge to move the legs starts or get worse during rest or inactivity
- The urge to move the legs is at least temporarily and partially or totally relieved by movements
- The urge to move the legs starts or is aggravated in the evening or in the night
- The criteria mentioned above are not due to any other behavioral or medical condition.
A doctor will first identify and focus on the individual’s descriptions of symptoms, their triggers, and relieving factors as well as the presence or absence of symptoms throughout the day. They may be a neurological and physical exam and take into account the person’s medical and family history and a list of current medications in order to diagnose this condition.
They may also be asked about the frequency, duration, and intensity of the symptoms, movements to relieve symptoms, the time it takes to fall asleep, any pain related to the symptoms, daytime sleeping patterns and sleepiness, disturbance of sleep, or daytime function. They may also conduct laboratory tests to rule out other conditions such as kidney failure, iron deficiency anemia, or pregnancy. Blood tests can also be conducted to check iron or any vitamin deficiencies.
In some cases, sleep studies such as polysomnography, that test the individual’s brain waves, heartbeat, breathing, and leg movements during an entire night. This test may help to identify the presence of any other sleep disorders that can be a cause of this condition.
The periodic limb movement of sleep during a sleep study can help to diagnose this condition. Diagnosing this condition in children can be tough since it may be hard for children to describe what they are experiencing, when and how often symptoms occur, and how long the symptoms last. Pediatric restless legs syndrome can be misdiagnosed as growing pains or attention deficit disorder.
Treatment For Restless Legs Syndrome
Research 10 Memon, M. D., Faiz, S., Zaveri, M. P., Perry, J. C., Schuetz, T. M., & Cancarevic, I. (2020). Unraveling the Mysteries of Restless Leg Syndrome. Cureus, 12(10), e10951. https://doi.org/10.7759/cureus.10951 shows that the condition is “progressive, and its prevalence increases with age.” This is why it is crucial to seek medical treatment. The primary aim of treatment is to ease the symptoms. The main form of treatment is with medications. Moving the affected limbs may give temporary relief. Symptoms can be controlled by finding and treating medical conditions such as peripheral neuropathy, diabetes, or iron-deficiency anemia. The treatment methods of this syndrome that are usually adopted include:
1. Lifestyle changes
There may be certain lifestyle changes that can help to provide some relief to some people. These changes include decreasing or avoiding consumption of alcohol and tobacco, maintaining a regular sleep pattern, exercising, massaging the legs, or taking a warm bath. There are new medical devices that are approved by the US Food and Drug Administration such as a foot wrap that puts pressure under the foot, or a pad that sends vibration at the back of the legs.
2. Medication And Supplements
Sometimes the patients are also prescribed medications to help minimize the symptoms. They include:
A. Iron supplements
People who have iron deficiency may also experience the symptoms of this condition. Hence, iron supplements are prescribed to maintain the balance of iron in the body. However, a common side effect of taking iron supplements is an upset stomach. Since iron is not absorbed properly into the body by the gut, it may cause constipation which can be treated with stool softeners such as polyethylene glycol. It is also found that some people don’t respond to iron supplements. Others may require an IV line to boost the iron deficiency in the body.
B. Anti-seizure or anticonvulsant drugs
The first line of treatment for RLS is anti-seizure medications. The Food and Drugs Administration (FDA) has approved medications such as gabapentin enacarbil 11 Kim ES, Deeks ED. Gabapentin Enacarbil: A Review in Restless Legs Syndrome. Drugs. 2016 May;76(8):879-87. doi: 10.1007/s40265-016-0584-1. PMID: 27146056. or pregabalin 12 Griffin E, Brown JN. Pregabalin for the Treatment of Restless Legs Syndrome. Ann Pharmacother. 2016 Jul;50(7):586-91. doi: 10.1177/1060028016643097. Epub 2016 Apr 18. PMID: 27091870. for treating moderate to severe RLS. This drug is found to be effective as dopaminergic treatment and there are no reports of symptoms getting worsened by this drug. The possible side effects include dizziness, fatigue, and sleepiness.
C. Dopaminergic agents
Dopaminergic agents are responsible for increasing dopamine. These medications are usually used to treat Parkinson’s disease. Symptoms were found to reduce when they were taken at night. The FDA approved medications include ropinirole, pramipexole, and rotigotine. The possible side effects of these drugs include nausea, dizziness, or other short term effects. Levodopa and carbidopa may be effective when used intermittently. According to a 2018 study 13 Kwatra, V., Khan, M. A., Quadri, S. A., & Cook, T. S. (2018). Differential Diagnosis and Treatment of Restless Legs Syndrome: A Literature Review. Cureus, 10(9), e3297. https://doi.org/10.7759/cureus.3297 , “Dopaminergic medications are one of the most widely studied and used therapies for RLS.”
Even though dopamine medications are effective, the symptoms may worsen when it is used on a long-term basis. The body tends to develop an increased tolerance which makes the medication less effective over time. These medications become less effective in the evening and the symptoms at night become more intense. The symptoms can even begin to affect the arms or trunk. However, these progressive worsening symptoms can be reversed by removing the individual from any dopamine-related medications.
The adverse effects of dopamine medication can include the development of impulsive or obsessive behaviors such as obsessive gambling or shopping.
D. Opioids
Drugs such as methadone, codeine, hydrocodone, or oxycodone can be prescribed to treat individuals with more severe symptoms of this condition. These are prescribed when the patient doesn’t respond to other medications. The possible side effects include constipation, dizziness, exacerbation of sleep apnea, and the risk of addiction. However, it has proven effective by taking very low doses.
E. Benzodiazepines
These drugs are responsible to help the patient have a restful sleep. However, if taken before bedtime they can sometimes cause daytime sleepiness, reduce energy and affect concentration. Benzodiazepines such as clonazepam and lorazepam are usually prescribed to treat anxiety, muscle spasms and insomnia. Since these drugs induce sleep apnea, it should not be prescribed to people with sleeping problems. “Benzodiazepines are drugs that can induce and maintain sleep and, hence, intuitively are thought to be beneficial to people with RLS,” explains a 2017 study 14 Carlos K, Prado GF, Teixeira CD, Conti C, de Oliveira MM, Prado LB, Carvalho LB. Benzodiazepines for restless legs syndrome. Cochrane Database Syst Rev. 2017 Mar 20;3(3):CD006939. doi: 10.1002/14651858.CD006939.pub2. PMID: 28319266; PMCID: PMC6464545. .
Recovery From Restless Legs Syndrome
This is a lifelong condition and there is no cure for this. Medications are prescribed to help ease or minimize the symptoms. Symptoms may gradually worsen with age or vice versa. The diagnosis of this condition doesn’t necessarily indicate the onset of any neurological disease such as Parkinson’s disease.
If the symptoms are mild and it doesn’t interfere with the individual’s sleep patterns, the condition does not have to be treated. It is important to seek medical attention if the symptoms are severe. With medication, it is possible to lead a quality life without any symptoms.
Restless Legs Syndrome At A Glance
- Restless legs syndrome is a nervous system disorder characterized by persistent and continuous urge to move one’s legs.
- Restless Legs Syndrome occurs when an individual experiences constant itchiness and discomfort in their legs, usually after going to bed.
- The primary symptom is an urge to move their legs.
- Women often experience the symptoms of this syndrome during pregnancy.











